 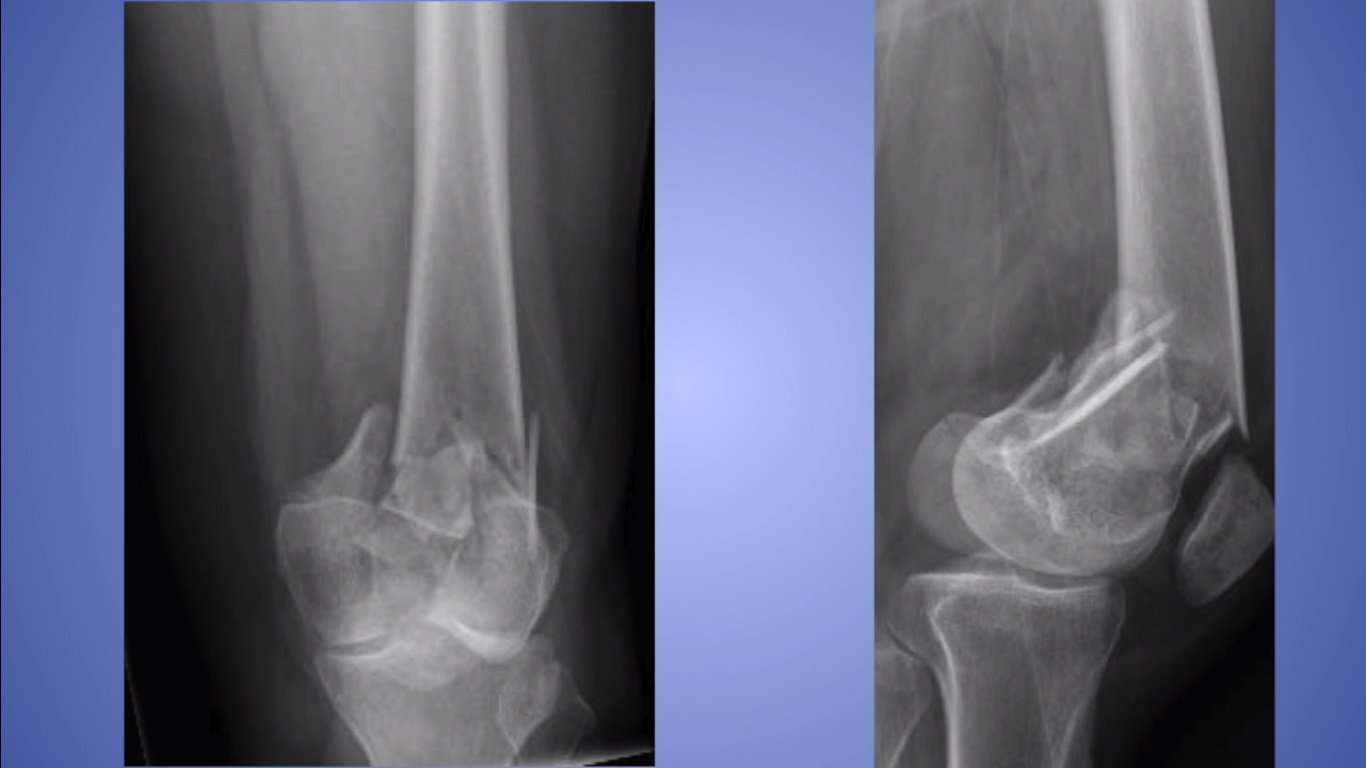 
However when it is so displaced by an effusion as to result in the ‘sail sign’ or when you see the posterior fat pad, it is a good marker for a fracture. You might normally see the anterior fat pad. If you can see a fat pad, it simply indicates a joint effusion. What are the X-ray Signs? The Fat Pad Sign HINT 1: If the patient presents with clinical signs of a fracture and the x-ray is normal, treat them like there is a fracture. A fracture can occur with a normal X-ray. The x-ray merely confirms that you have found it. 30 Consequently, fractures in the intracapsular region have a higher incidence of avascular necrosis, nonunion or malunion, and degenerative changes.How good are you at reading elbow X-rays? Here are some tools and rules that will help you pick up those elbow fractures.įractures of the elbow usually fall into the following groups:įractures are a CLINICAL Diagnosis. The femoral neck region has a thin periosteum, little cancellous bone, and a relatively poor blood supply. Subtrochanteric fractures, however, have an increased need for intramedullary rods or nails (impact devices) and have a higher rate of impact failure, mainly because of the high stresses on this part of the femur. 30 As a result, fractures in this region typically heal well with open reduction and internal fixation, which involves surgery to reduce the displaced bone, followed by internal fixation of the fracture with plates or screws. 30 The intertrochanteric region contains a large amount of cancellous bone and an adequate blood supply. The two categories are extracapsular (intertrochanteric and subtrochanteric) and intracapsular (femoral head and neck) these are summarized in Table 2. Hip fractures are classified by location for prognostic implications. Some patients may benefit from a fall-prevention assessment. 
Unless contraindicated, bisphosphonate therapy should be used to reduce the risk of another hip fracture. Rehabilitation is critical to long-term recovery. In addition, patients should receive thromboembolic prophylaxis, preferably with low-molecular-weight heparin. Patients should receive prophylactic antibiotics, particularly against Staphylococcus aureus, before surgery. The consulting orthopedic surgeon will choose the surgical procedure. Most fractures are treated surgically unless the patient has significant comorbidities or reduced life expectancy. If an occult hip fracture is suspected and plain radiography is normal, magnetic resonance imaging should be ordered. Plain radiography with cross-table lateral view of the hip and anteroposterior view of the pelvis usually confirms the diagnosis. During the physical examination, displaced fractures present with external rotation and abduction, and the leg will appear shortened. Patients with hip fractures have pain in the groin and are unable to bear weight on the affected extremity. Most hip fractures are associated with a fall, although other risk factors include decreased bone mineral density, reduced level of activity, and chronic medication use. Women experience 80% of hip fractures, and the average age of persons who have a hip fracture is 80 years. Hip fractures cause significant morbidity and are associated with increased mortality. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
